
Surprisingly, rosacea (and often couperose) is not always a matter of collagen synthesis, genetics, photosensitivity, or frequent visits to a cosmetologist. Rosacea results from a combination of dysregulated immune system signaling, abnormal neurological and vascular responses, and dysbiosis of microorganisms, leading to skin sensitivity and inflammation.
Innate Immune System
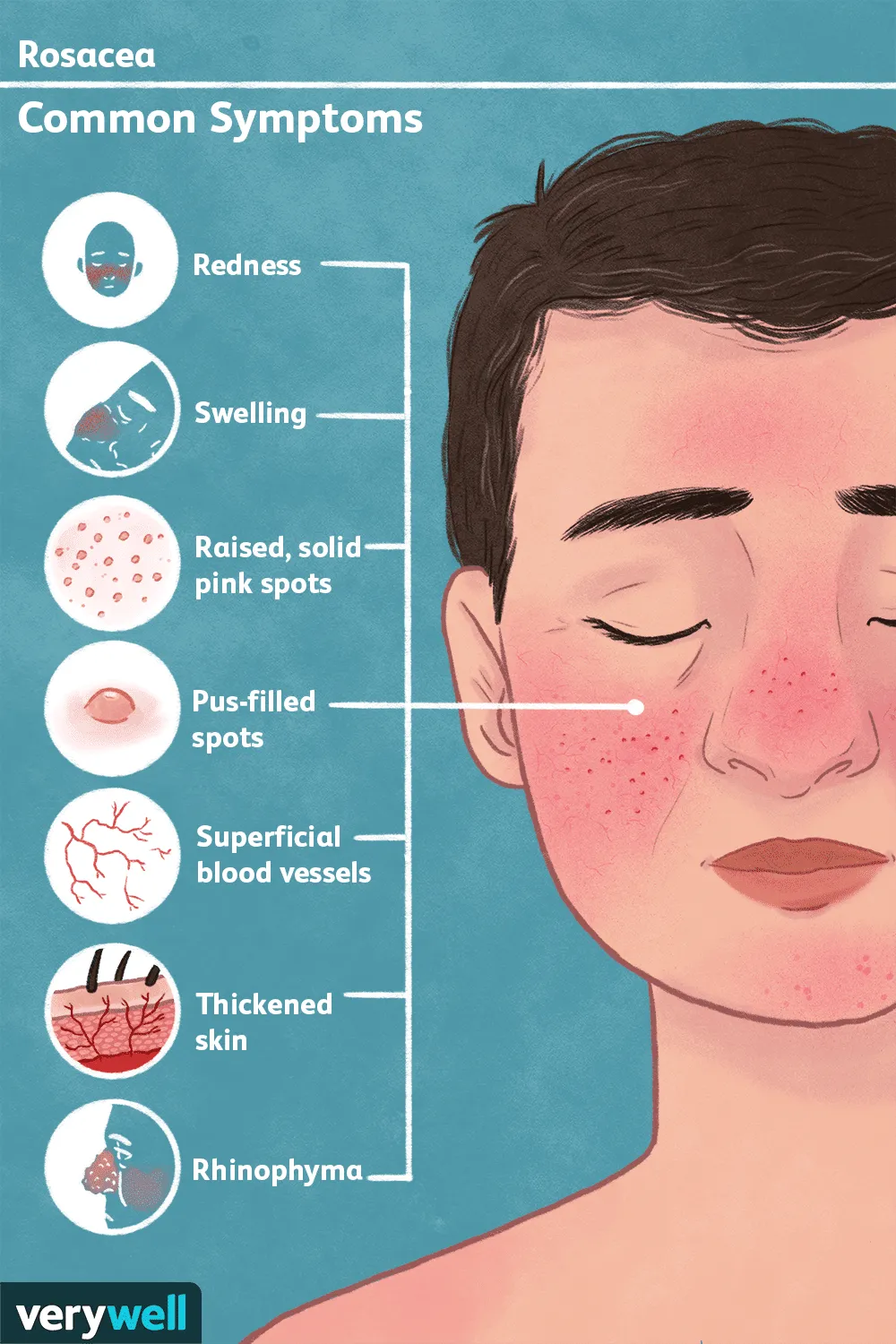
In rosacea, the innate immune system is disrupted, characterized by abnormal release of inflammatory peptide molecules that are intended to protect against bacteria.
Abnormal Neurological Signaling
Triggers like heat, abrupt environmental changes, certain foods (alcohol, tea, coffee, cocoa, chocolate, spices, citrus fruits, tomatoes, cinnamon — not to be confused with allergies or intolerances), as well as emotions like anger or embarrassment, activate inflammatory cascades via sensory nerves. Melanocytes (pigment cells) originating from the neural crest initiate vascular signaling in this process.
Bacteria and Mites
- Direct involvement: Staphylococcus epidermidis, Demodex, Bacillus oleronius.
- Indirect involvement: Escherichia coli, Helicobacter pylori.
Conditions like SIBO, IBS, and IBD (especially undiagnosed or chronic gastrointestinal diseases) contribute to microbial dysbiosis.
Even in healthy individuals, the skin reflects gastrointestinal health in 90% of cases. When flare-ups occur, consider the following:
- Liver enzymes and bile function (seborrheic dermatitis and flaking may also point to this).
- Adequate stomach acid levels (bile and gastric juice act as natural disinfectants; if they are impaired, gut microbiota and intestinal integrity suffer).
- Address underlying conditions like gastritis, duodenitis, cholecystitis, pancreatitis, etc.
- Healthy gut flora (without excessive pathogens, fungi, or issues like thrush and cystitis — treat the flora, and your skin will improve).
- Pseudoallergic reactions (xenobiotics, histamine, gluten, dairy proteins).
- Presence or absence of autoimmune diseases.
Recent exacerbations are often tied to ineffective digestion under stress and imbalanced diets. Today, the GI tract is a therapeutic target.
The Connection Between Gut Dysbiosis and Rosacea
Gut bacterial dysbiosis activates the kallikrein-kinin pathways in plasma, leading to neurogenic inflammation.
Key Steps to Manage Rosacea
- Treat Inflammation and Address Congestion
Eliminate existing inflammation and resolve any stagnation in the body. - Support a Healthy Microbiome
The gut microbiota plays a crucial role in skin health.- Prebiotics: flaxseed, greens, chicory, psyllium, onions, garlic, cold potatoes, sweet potatoes, sesame seeds, mushrooms, Jerusalem artichokes, and adequate dietary fiber.
- Probiotics: fermented foods like sauerkraut, kombucha, miso, yogurt, kefir from whole milk, symbiotics in supplements, and postbiotics. Specific strains should only be recommended by professionals.
- Omega-3 Fatty Acids with EPA Dominance
- Zinc (Sulfate or Picolinate)
Use it short-term as excessive use may deplete other metals. - Eliminate Individual Food Triggers and Inflammatory Foods
Refined grains, sugar, milk, and artificial sweeteners should be avoided. - No Specific Diet Exists
Focus on treating inflammation in the body and feeding the microbiota with a balanced, healthy diet. - Regular Bowel Movements
Going to the toilet less than once a day is not normal. - Antibiotic Therapy as a Gold Standard
This is used when the cause is bacterial overgrowth. However, its effectiveness varies, often causing relapses and significant microbiota disruption. Herbal concentrates (natural antibiotics) may be a better alternative, including eleutherococcus, garlic extract, grapefruit seed extract, berberine, oregano oil, and wormwood. - Other Diets, Exclusions, and Protocols
These should be determined by a nutritionist, immunologist, dermatologist, dietitian, or gastroenterologist.



